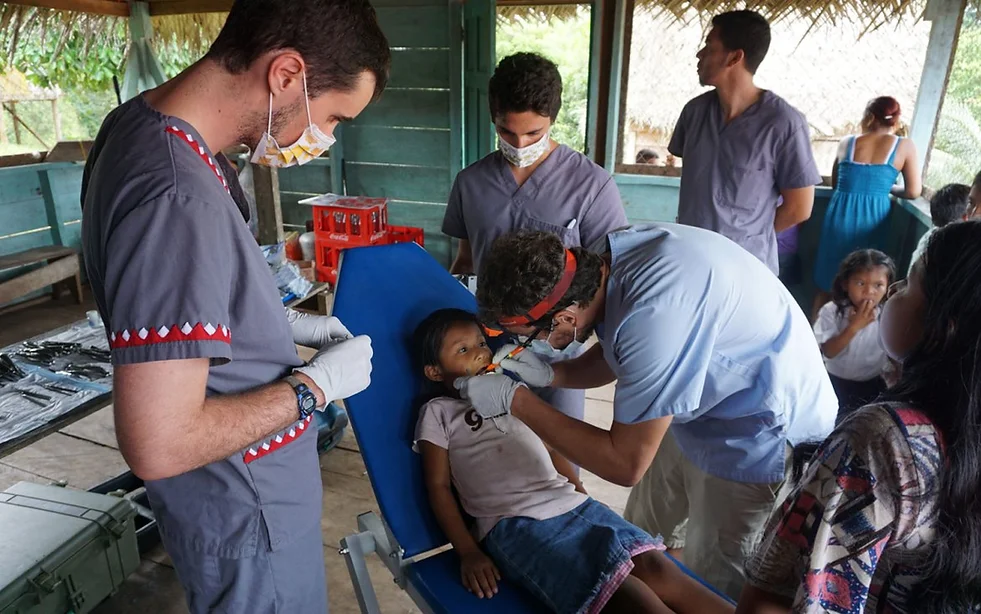
Specialties in Remote Settings
Discount
full course bundle
Credits
AMA PRA Category 1 Credits™
Course Duration
10 hours and 15 minutes total
Instructors
Dr. George LaBrot
Learn how to be a specialist during medical missions
ACCME Accreditation Statement:
Lesson Plan
Mental Health in Resource-Limited Settings | 65 minutes
Infectious Disease in Underserved Regions | 26 minutes
Gastrointestinal Issues in Developing World Settings | 39 minutes
Tropical Dermatology | 64 minutes
Cardiology in Mission Settings | 53 minutes
Neurology | 70 minutes
Respiratory Medicine in Mission Settings | 73 minutes
Orthopedics & Other Musculoskeletal Issues | 55 minutes
Allergies | 25 minutes
Endocrinology in Underserved Settings | 41 minutes
Genitourinary & Breast Health | 49 minutes
Geriatrics and End of Life Care | 56 minutes
Dr. Benjamin LaBrot
Dr. Benjamin LaBrot is a career medical missionary and the founder of the Floating Doctors medical team, specializing in sustainable health access improvements in challenging rural environments. He received his medical training at the Royal College of Surgeons in Ireland, and practiced for many years in the Irish Health Care System, where he assisted in setting up a long-term care elderly facility. (Ben or Dr. LaBrot) currently splits his time working with Floating Doctors and teaching as a Clinical Assistant Professor of Medical Education at the Keck School of Medicine of the University of Southern California.
Dr. George LaBrot
Dr. LaBrot is a patient-centered physician who values the long-term relationships he has established with so many patients over the years. He has a broad range of medical knowledge, having been Board Certified four times in Internal Medicine, Pulmonary Disease, Critical Care and Sleep Medicine. Dr. Labrot earned his medical degree from the University of Illinois at Chicago College of Medicine. He has traveled the world treating patients in resource limited areas of the world, including working with Mother Teresa in Calcutta, India. He is a popular lecturer for the University of Minnesota biannual CME program in Delivery of Medical Care in Resource Poor Areas.
